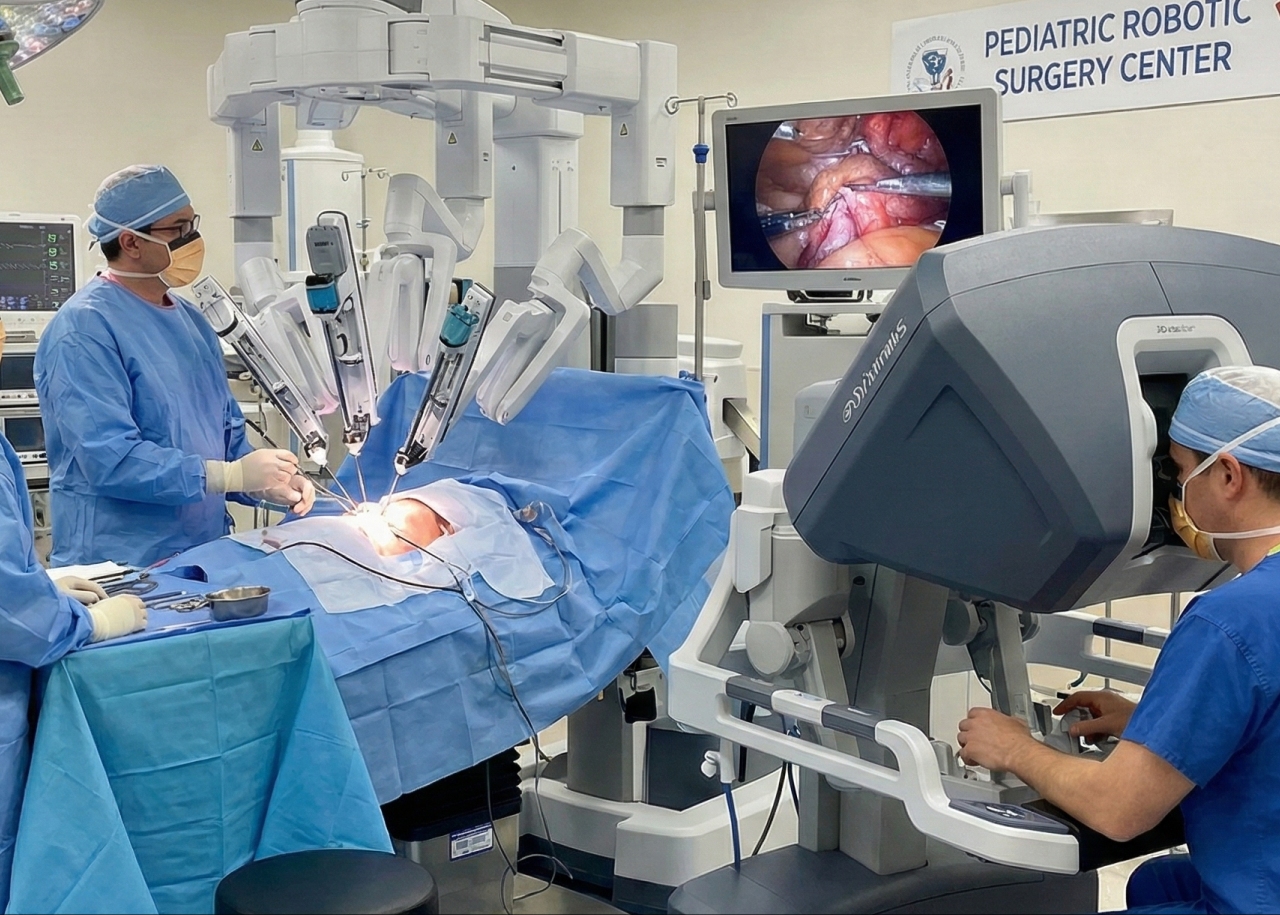
In a landmark achievement for pediatric surgery in the UAE, a 14-year-old girl became the first child in the country to undergo robotic spleen-sparing distal pancreatectomy. The complex procedure, performed at Burjeel Medical City, demonstrates the advancement of minimally invasive pediatric surgery and the expertise now available locally for the most challenging cases.
The Discovery
The teenager presented with a history of recurrent upper abdominal pain. Initial evaluation and imaging revealed an unexpected finding: a cystic mass of the pancreas requiring specialized surgical intervention.
Comprehensive Investigation
Laboratory Tests: All routine labs were normal
Ultrasound:
- Well-defined hypoechoic lesion medial to left lobe of liver
- Located in gastro-hepatic region
- Abutting the body of pancreas
CT Scan:
- Well-defined hypodense mass (46×44 mm)
- Located in distal body of pancreas
- No significant enhancement
- No calcification
- No pancreatic duct dilatation
- Normal peri-pancreatic tissues
MRI Pancreas:
- 45 x 44 x 38 mm well-circumscribed enhancing lesion
- Distal body of pancreas
- Intralesional hemorrhagic component
- Diagnosis suggested: Solid pseudo-papillary epithelial neoplasm (SPEN)
EUS with FNA:
- Endoscopic ultrasound with fine needle aspiration
- Confirmed diagnosis: SPEN
Understanding SPEN
Solid Pseudo-Papillary Epithelial Neoplasm (SPEN):
- Rare type of pancreatic cystic neoplasm
- Low malignant potential
- Predominantly affects young females (90% of cases)
- Usually asymptomatic
- Can grow to large size
- May produce vague symptoms
- If at pancreatic head: can cause jaundice
Natural History:
- Slow-growing tumor
- Can reach significant size
- Pressure effects on nearby structures
- Excellent prognosis with complete surgical removal
- Very low recurrence rate after complete resection
The Surgical Decision
Given the tumor’s nature and potential to grow, early surgical treatment was advised. The planned approach: minimally invasive distal pancreatectomy with spleen preservation using robotic technology.
Why preserve the spleen?
- Spleen is vital for immune function
- Protects against certain bacterial infections
- Particularly important in children and young adults
- Removal increases lifelong infection risk
- Preservation significantly beneficial
Why robotic surgery?
- Enhanced precision in tight anatomical spaces
- 3D high-definition visualization
- Wristed instruments allow delicate dissection
- Preserves delicate splenic blood vessels
- Faster recovery than open surgery
- Better cosmetic outcome
- Reduced post-operative pain
The Complex Surgical Challenge
Spleen-sparing distal pancreatectomy is one of the most technically demanding pancreatic operations:
Anatomical Complexity:
- Splenic artery and vein course through entire pancreas length
- Vessels intimately attached to pancreatic tissue
- Multiple small branches supply spleen
- Separating vessels from pancreas requires extreme precision
Surgical Precision Required:
- Individual ligation of pancreatic branches
- Preservation of all splenic vessel branches
- Avoiding vessel injury (causes uncontrolled bleeding)
- Preventing vessel spasm (compromises spleen)
- Complete tumor removal with margins
- Minimizing blood loss
Pediatric Specific Challenges:
- Small body size limits working space
- Delicate tissues require gentle handling
- Lower blood volume—minimal loss tolerance
- Psychological considerations for teenager
- Family anxiety management
The Robotic Advantage
The Da Vinci Robot provided critical advantages:
Visualization:
- 10x magnification
- 3D high-definition imaging
- Superior to human eye and 2D laparoscopy
Instrumentation:
- Wristed instruments (7 degrees of freedom)
- Tremor elimination
- Scaled motion (surgeon’s hand movements reduced)
- Precise dissection in millimeters
Ergonomics:
- Surgeon at comfortable console
- Reduced fatigue during long procedures
- Maintains precision throughout operation
- Better decision-making
The Procedure
Operative Approach:
- Patient positioned appropriately
- Robotic ports placed
- Da Vinci Xi system docked
- Systematic approach to pancreatic mobilization
- Careful dissection of splenic vessels
- Distal pancreatectomy performed
- Spleen preserved with intact blood supply
- Hemostasis achieved
- No drain required (per ERAS protocol)
Enhanced Recovery After Surgery (ERAS) Protocol:
- No drain tubes
- No urinary catheter
- No gastric tubes
- Early mobilization
- Early oral intake
- Reduced opioid use
- Faster discharge
Operative Results:
- Successful complete tumor removal
- Spleen fully preserved
- Minimal blood loss
- No complications
- Excellent hemostasis
Remarkable Recovery
Post-Operative Day 1 (POD 1):
- Mobilized after 6-8 hours
- Tolerated oral liquids after 8 hours
- Pain adequately controlled
- No ICU stay required
- Shifted to regular ward
POD 3:
- Reached full oral feeds
- Walking independently
- Minimal pain
- Normal bowel function
POD 7:
- Cleared for discharge
- Eating regular diet
- No restrictions
- Follow-up scheduled
Pathology Results
Histopathology confirmed: Solid pseudo-papillary epithelial neoplasm
- Complete removal achieved
- Clear margins (R0 resection)
- No malignant features
- Excellent prognosis
Why This Surgery Matters
For the Patient:
- Tumor removed completely
- Spleen preserved (lifelong immune benefit)
- Minimal scarring (4 small incisions)
- Fast recovery (7 days hospital)
- Returned to school quickly
- Normal teenager life resumed
For the Region:
- First pediatric robotic pancreatic surgery in UAE
- Previously required travel abroad
- Local expertise now available
- Family stays together
- Cost-effective quality care
- Establishes program for future cases
For Burjeel Medical City:
- Demonstrates advanced capabilities
- Pediatric robotic surgery program
- Multidisciplinary excellence
- International-standard outcomes
- Regional referral center status
The Multidisciplinary Approach
Success required collaboration across specialties:
- Gastroenterology: Diagnosis and EUS-FNA
- Radiology: Detailed imaging interpretation
- Pediatric Surgery: Surgical expertise
- Anesthesia: Pediatric robotic anesthesia management
- Pathology: Frozen section and final diagnosis
- Nutrition: Post-operative dietary management
- Nursing: Specialized pediatric surgical care
Long-Term Prognosis
With complete SPEN removal:
- Cure rate: >95%
- Recurrence: very rare
- Normal pancreatic function expected
- Preserved spleen function
- No dietary restrictions
- Regular surveillance only
- Excellent quality of life
- Normal life expectancy
Burjeel’s Robotic Surgery Excellence
Da Vinci Xi Capabilities:
- Latest generation robotic system
- Pediatric and adult applications
- Multiple surgical specialties
- Experienced robotic surgeons
- High-volume robotic program
- Superior outcomes
- Comprehensive training program
Specialties Using Robotics:
- Gastrointestinal surgery
- Urology
- Gynecology
- Thoracic surgery
- Cardiac surgery
- Pediatric surgery
Our Experts

Dr. Ali Iyoob Valiyaveettil
Consultant and Head – Gastro-Intestinal Surgery
Burjeel Medical City, Abu Dhabi

Advanced Pediatric & Robotic Surgery
Complex pediatric conditions require specialized expertise and child-focused care. Our robotic surgery program provides comprehensive evaluation and advanced minimally invasive solutions for children and adolescents.